Endocrine Pathology
4
Products
Multinodular goitre
Clinical HistoryA 53-year-old female presented with an abnormal neck swelling and persistent cough. She also experienced lethargy and weight gain over several years. During investigations, she died months later from unrelated cardiovascular disease.Pathology The post-mortem specimen includes the base of the tongue, larynx, and trachea. The thyroid gland is grossly enlarged, especially the right lobe, extending beyond its normal boundaries. The cut surfaces show multiple hyper- and hypopigmented nodules and cystic areas in both lobes. The tongue base, larynx, and trachea appear normal.Further InformationNodular goitre is usually detected as a neck swelling. Depending on size and location, it can cause pressure symptoms like difficulty breathing, dysphagia, cough, or hoarseness. Rarely, recurrent laryngeal nerve paralysis occurs. Sudden growth or tenderness can result from cystic expansion or hemorrhage within nodules.Causes include autoimmune diseases (Hashimoto’s thyroiditis, Grave’s disease), thyroid nodules, and iodine deficiency. Goitre develops when thyroid hormone synthesis is reduced—due to biosynthetic defects or iodine shortage—leading to increased TSH stimulation and thyroid growth. In Hashimoto’s, elevated TSH combined with fibrosis enlarges the thyroid. In Grave’s disease, stimulation by TSH receptor antibodies causes the goitre.
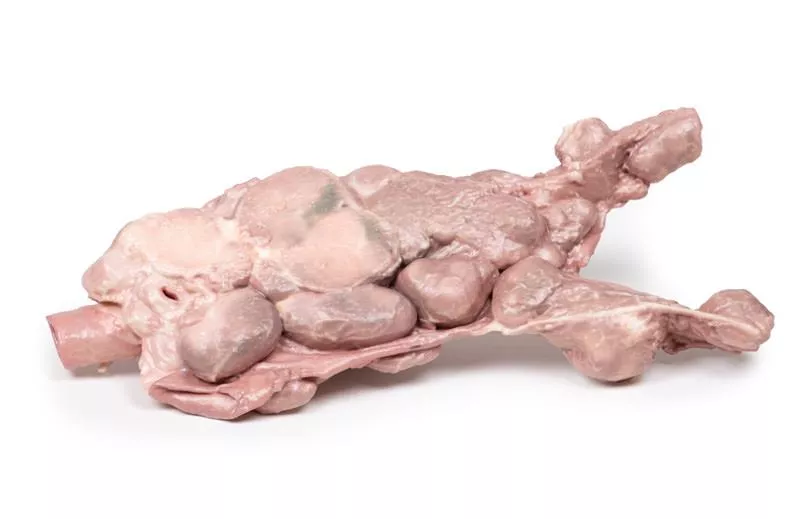
Retrosternal Goiter
Clinical HistoryA 60-year-old woman presented with an abnormal swelling in her neck, a persistent cough, and difficulty swallowing. Over the previous years, she had experienced weight gain. She later died of an unrelated cardiovascular condition, and the specimen was collected during the post-mortem examination.PathologyThe post-mortem specimen includes the larynx, trachea, and a large, multilobular thyroid gland. The thyroid is significantly enlarged, especially the right lobe, which features two prominent lobes extending 7–8 mm superiorly and inferiorly—well beyond normal boundaries from the front view. Posteriorly, the oesophagus has been opened to show the rear wall of the trachea. The right lobe appears even larger from this angle, with the abnormal growth concentrated at its inferior pole. No major pigmentation changes are observed on the surfaces, but prominent veins are visible on the right lobe.Further InformationGoitre often presents as a visible neck swelling. Depending on its size and location, it may cause pressure symptoms such as difficulty breathing, swallowing issues (dysphagia), hoarseness, and persistent cough. In rare cases, an expanding goitre can paralyse the recurrent laryngeal nerve. Symptoms of tracheal obstruction, including stridor and shortness of breath, may occur. Sudden tenderness and rapid enlargement may result from cystic expansion or bleeding into a thyroid nodule.Common causes of goitre include autoimmune diseases (such as Hashimoto’s thyroiditis and Grave’s disease), thyroid nodules, and iodine deficiency. Goitre usually results from reduced thyroid hormone synthesis due to biosynthetic defects or iodine deficiency. This leads to increased TSH (thyroid-stimulating hormone), which stimulates thyroid growth in compensation. In Hashimoto’s thyroiditis, elevated TSH and autoimmune-related fibrosis both contribute to gland enlargement. In Grave’s disease, thyroid growth is primarily driven by TSH receptor antibodies.Reference: Hughes et al. (2012). Goitre: Causes, investigation and management. Aust Family Physician, 41, 572–576.
Aorta & para-aortic lymph nodes
Clinical HistoryThis case involves a 75-year-old woman who presented with recurrent symptoms five years after initial treatment for stage IIIc serous adenocarcinoma of the ovary. She was diagnosed with chemo-resistant retroperitoneal lymph node metastases, involving both para-aortic and pelvic nodes, as shown on PET/CT imaging. Unfortunately, she died of liver complications before options like radical lymphadenectomy could be explored.PathologyThe specimen includes the abdominal aorta and common iliac arteries, surrounded by a large number of enlarged para-aortic and iliac lymph nodes. Histopathological analysis confirmed metastatic high-grade adenocarcinoma in several of these nodes.Further InformationIn some cases of recurrent ovarian cancer, lymph node metastases may be the only sign of disease. In this patient, PET/CT findings accurately predicted all metastatic nodes. While ultrasound (US) could have also detected the enlarged nodes, both PET/CT and US may miss microscopic disease, making it difficult to fully exclude lymph node involvement during follow-up.In younger women with recurrent ovarian cancer but no other spread, systematic dissection of aortic and pelvic nodes may offer symptom relief and open the door for novel therapies, although it is rarely curative.More typically, pelvic and aortic lymph node sampling forms part of initial surgical staging in epithelial ovarian cancer. For women with advanced-stage disease, surgical removal of enlarged retroperitoneal lymph nodes may be appropriate if it enables complete tumour debulking.
Lymphoma of the thyroid
Clinical HistoryA 68-year-old woman presented with a small, hard thyroid lump. Over six weeks, the mass rapidly enlarged, causing laryngeal stridor and oesophageal obstruction. No lymphadenopathy or splenomegaly was noted.Pathology The specimen includes the larynx, thyroid, upper trachea, and oesophagus. The enlarged left thyroid lobe, and to a lesser extent the right, is replaced by homogeneous pale tumour tissue. The tumour compresses the larynx and oesophagus. Histology confirmed lymphoblastic lymphoma of the thyroid. Due to its rarity, anaplastic carcinoma and secondary lymphoma spread must be excluded.Further InformationPrimary thyroid lymphoma is rare but important to consider in thyroid masses. Most are non-Hodgkin lymphomas; lymphoblastic lymphoma is aggressive and usually seen in children. The main known risk factor is chronic autoimmune (Hashimoto’s) thyroiditis, present in about 50% of cases.Over 90% of patients present with a rapidly enlarging goitre causing compression of trachea, oesophagus, and neck vessels, resulting in symptoms like stridor, hoarseness, dysphagia, and neck pain. Systemic ‘B-symptoms’ may include night sweats, fever, and weight loss.Diagnosis requires ultrasound with fine needle aspiration or biopsy. Cytology and immunohistochemistry are essential to differentiate lymphoma from Hashimoto’s thyroiditis or carcinoma.
Human body replicas to improve teaching!
Erler-Zimmer's groundbreaking Anatomy Series features a unique and unrivalled collection of colourised human body replicas specifically designed to enhance teaching and learning. This premium collection of highly accurate human anatomy has been created directly from radiological data or real specimens using the latest imaging techniques. The 3D Human Anatomy Series offers a cost-effective way to meet your specific teaching and demonstration needs across the curriculum in medicine, health sciences and biology. A detailed description of the anatomy represented in each 3D printed specimen is included. What are the advantages of the Monash 3D Anatomy Series compared to plastic models or real human plastinates?
Each body replica has been carefully developed from selected radiological patient data or dissected human bodies of the highest quality, chosen by a highly skilled team of anatomists at Monash University's Human Anatomy Teaching Centre, to represent clinically important areas of anatomy in a quality and detail not possible with conventional models - it is real anatomy, not stylised. Each body replica has been rigorously checked by the highly qualified team of anatomists at Monash University's Human Anatomy Teaching Centre to ensure the anatomical accuracy of the final product. The body replicas are not real human tissue and are therefore not subject to any restrictions on transport, import or use in educational institutions that do not have permission to use cadavers. The
exclusive 3D Anatomy Series avoids these and other ethical issues that arise when dealing with plastinated human remains.