Brain pathology
19
Products
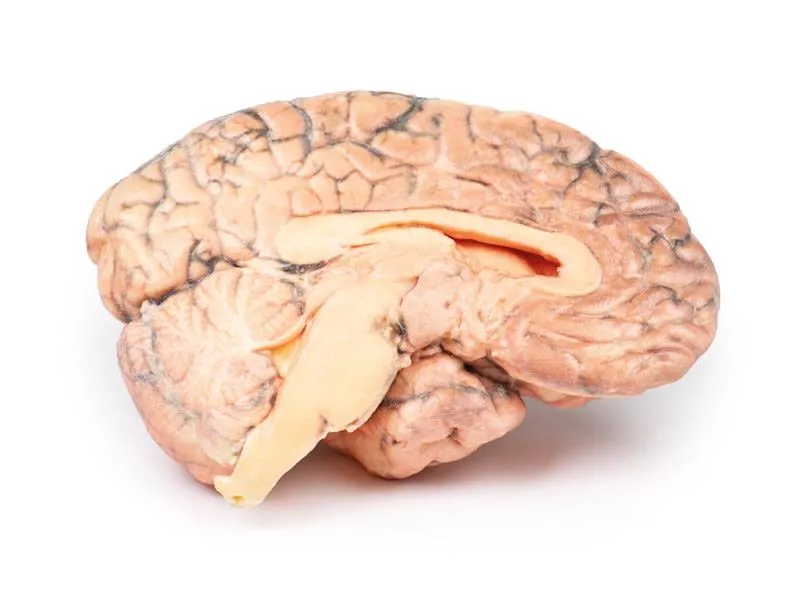
Cerebral Haemorrhage
Clinical HistoryA 56-year-old woman was admitted after two episodes of severe headache accompanied by loss of consciousness. Examination revealed systemic hypertension, cardiac enlargement, and right-sided hemiparesis. Angiography detected bilateral middle cerebral artery aneurysms. Her condition rapidly worsened, and she died shortly after admission.PathologyThe left cerebral hemisphere, sectioned parasagittally, shows a large cerebral haemorrhage involving the parietal and frontal lobes. The haemorrhage and associated clot have significantly distorted the external capsule and lateral ventricle. The bleeding originated from a ruptured aneurysm of the left middle cerebral artery.
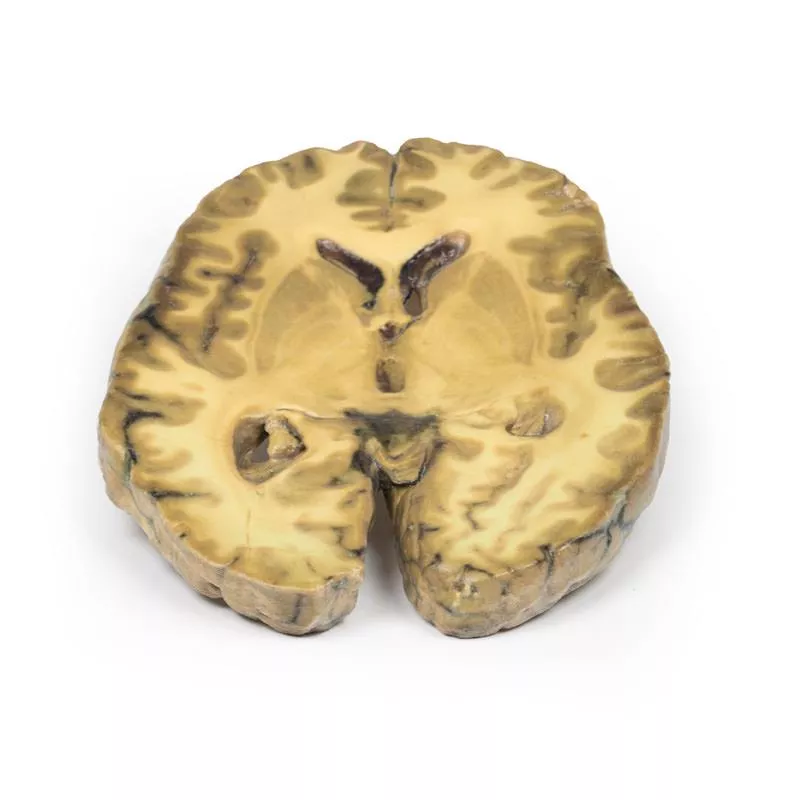
Intracerebral Haemorrhage
Clinical HistoryAn 80-year-old man suddenly lost consciousness. On examination, there was a right gaze palsy, left hemiplegia, and right hemiparesis.Pathology Coronal sections at the level of the mammillary bodies, including the brainstem and anterior temporal lobes, show a massive clot replacing tissue in the left basal ganglia and internal capsule. The haemorrhage ruptured into the left lateral ventricle and temporal horn, destroying its walls and infiltrating adjacent brain. The right lateral ventricle is also filled with blood but retains intact walls. The clot acts as a space-occupying lesion, expanding the left hemisphere and shifting midline structures rightward. A subfalcine herniation of the left cingulate gyrus under the falx cerebri is evident. Further Information Intracerebral haemorrhages of this type commonly result from systemic hypertension. The bleed arises from the rupture of a micro-aneurysm in striate artery branches supplying the basal ganglia.
Ruptured Berry Aneurysm
Clinical History A 38-year-old woman developed sudden pain behind the right eye, followed by progressive weakness of the left leg. On examination, she was confused and hypertensive with left-sided hemiparesis, right homonymous hemianopia, and a right VIth cranial nerve palsy. Reflexes were brisk on the left side, with an upgoing plantar reflex. Lumbar puncture revealed raised pressure and blood-stained CSF. Angiography identified an intracerebral aneurysm, which was clipped surgically. Unfortunately, the patient died suddenly the day after surgery.Pathology The basal brain surface shows a 5 mm saccular aneurysm at the junction of the right internal carotid and posterior communicating artery, which had ruptured. Subarachnoid haemorrhage is visible in the cisterna magna and on the inferior right frontal lobe. A similar unruptured aneurysm is also present on the left. The right frontal lobe appears soft and friable. Further Information Posterior communicating artery aneurysms are the third most common among Circle of Willis aneurysms and can compress nearby cranial nerves, such as the abducens (VI). The patient’s retro-orbital pain may relate to irritation of the trigeminal nerve, while the visual field defect likely resulted from pressure on the right optic tract. Neurological symptoms depend on the affected vascular territory of the cerebral cortex.
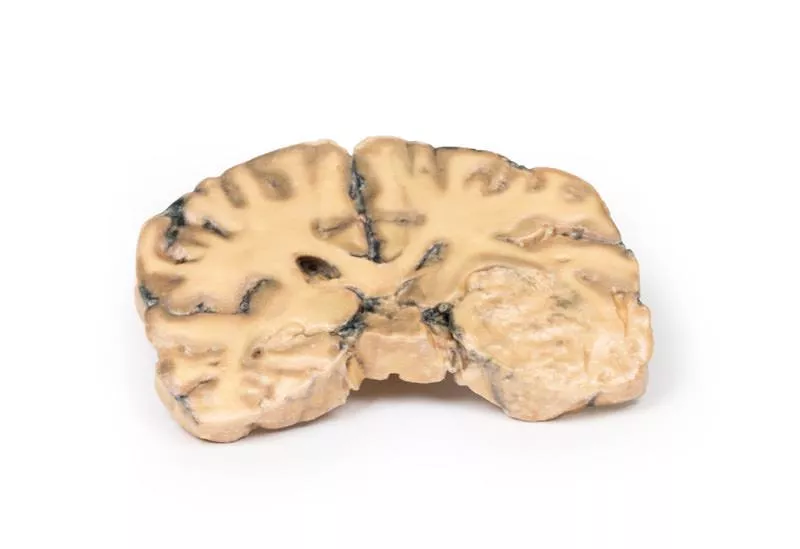
Astrocytoma
Clinical HistoryA 73-year-old woman was admitted with new left-sided hemiplegia. On further questioning, she reported a 3-month history of headaches, nausea, and worsening balance. CT identified an inoperable brain tumour. She passed away one week after admission.Pathology A coronal brain slice reveals a poorly demarcated tumour in the right temporal lobe, causing hemispheric enlargement and flattening of the gyri. The posterior view shows subfalcine herniation, and the mass displays areas of necrosis and haemorrhage. Histology confirmed an astrocytoma, Grade III/IV. Further InformationAstrocytomas are a subtype of glioma, the second most common CNS cancer after meningioma. Originating from astrocytes, they are classified by grade—diffuse (II), anaplastic (III), to glioblastoma (IV). Typical histology shows gemistocytes with eosinophilic cytoplasm against a fibrillary background. Most occur in the hemispheres of patients aged 40–60 and present with seizures, headaches, nausea, or focal deficits. Without treatment, median survival for Grade III tumors is ~~18 months. Management involves surgery, radiotherapy, chemotherapy, or combinations tailored to the patient.
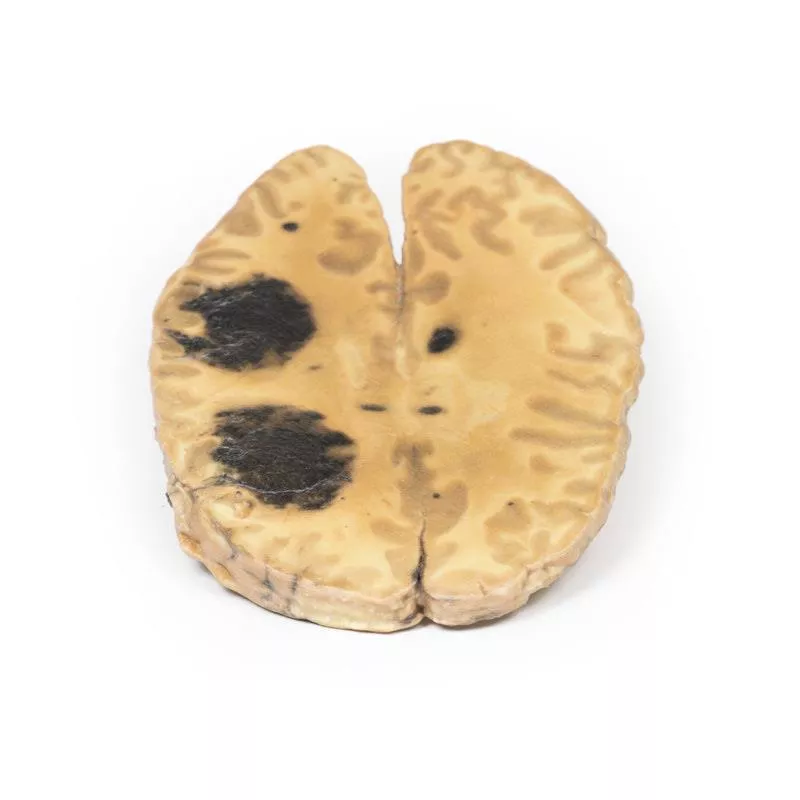
Metastatic melanoma
Clinical HistoryIn the 1970s, a 31-year-old woman presented with severe headache and diplopia, eight months after the removal of an invasive pigmented skin melanoma from her neck. Initial clinical examination revealed no abnormalities. She was discharged but re-admitted later with persistent vomiting. Her condition rapidly deteriorated, and she died shortly after.PathologyThe brain specimen shows extensive intracerebral melanoma metastases. The inferior surface displays numerous dark nodules up to 1.5 cm in diameter. On the cut superior surface, similar lesions are visible and confined to the grey matter. The tumour nodules are not encapsulated and infiltrate the cortex, with areas of necrosis and haemorrhage present. Further InformationMelanoma accounts for about 10% of all brain metastases. Risk increases with age over 60, male gender, disease progression, and certain genetic mutations such as BRAF or NRAS. Most metastases are supratentorial and may present with headache, neurological deficits or seizures. These lesions have a known risk of spontaneous haemorrhage. Diagnosis is based on imaging and histological confirmation. Treatment often involves stereotactic radiosurgery, radiotherapy, and systemic immunotherapy or targeted therapies, improving median survival to around 11 months in recent years.
Metastatic carcinoma in the brain
Clinical HistoryThis 51-year-old woman had undergone surgery for breast carcinoma two years before presenting with left-sided ataxia of two weeks’ duration. A previous fainting episode followed by weakness on the same side had preceded this. Examination revealed left spastic paresis. Due to the rapid onset of symptoms, a vascular lesion was suspected. Despite discharge, she was re-admitted six weeks later with left-sided seizures. Lumbar puncture and clinical re-evaluation were inconclusive, but EEG showed a right anterior temporal abnormality. Angiography then revealed a large space-occupying lesion in the right cerebrum. Her condition continued to deteriorate, ultimately resulting in death.PathologyThe horizontal brain slice reveals three cystic tumours, predominantly in the right parietal region. The largest measures 5 cm in diameter. Another tumour is seen near its posterior margin, and a third, smaller one is found in the left parietal region. The tumours mainly affect the white matter, with shaggy, friable greyish tissue walls. The largest tumour had ulcerated into the right lateral ventricle, and subfalcine herniation with displacement of the basal ganglia and internal capsule was observed. Histology confirmed metastatic carcinoma. Additional metastases were found in the liver and bone, consistent with a primary breast carcinoma.
Glioblastoma multiforme
Clinical HistoryA 56-year-old male presented with a generalised seizure after which he remained unconscious and later died. A history revealed 6 months of progressive confusion, short-term memory loss, and personality changes.PathologyPost-mortem coronal brain sections show a 4 cm necrotic and haemorrhagic tumour invading from the inferior frontal lobe into the lateral ventricle. Meningeal spread is visible on the posterior aspect. Further InformationGliomas are the second most common central nervous system cancers after meningiomas. They originate from glial-like cells such as astrocytes, oligodendrocytes, or ependymal cells. Glioblastoma multiforme (GBM), a grade IV astrocytoma, arises from astrocytes and may develop de novo or from lower-grade tumours. GBMs typically show necrosis surrounded by anaplastic cells and hyperplastic blood vessels. More frequent in males, GBM commonly occurs in the 6th decade. Risk factors include neurofibromatosis type 1, Li-Fraumeni syndrome, and prior brain radiotherapy. Symptoms depend on tumour location and include persistent headaches, visual disturbances, vomiting, appetite loss, mood and personality changes, cognitive decline, seizures, and speech difficulties. Diagnostic tools are CT and MRI. About 50% of GBMs involve more than one hemisphere, often invading ventricles or meninges, with rare spinal cord spread. Metastasis outside the CNS is uncommon. Tumour growth leads to cerebral oedema and increased intracranial pressure. These aggressive tumours have a median survival of approximately 3 months if untreated. Treatment consists of surgery followed by radiation and chemotherapy.
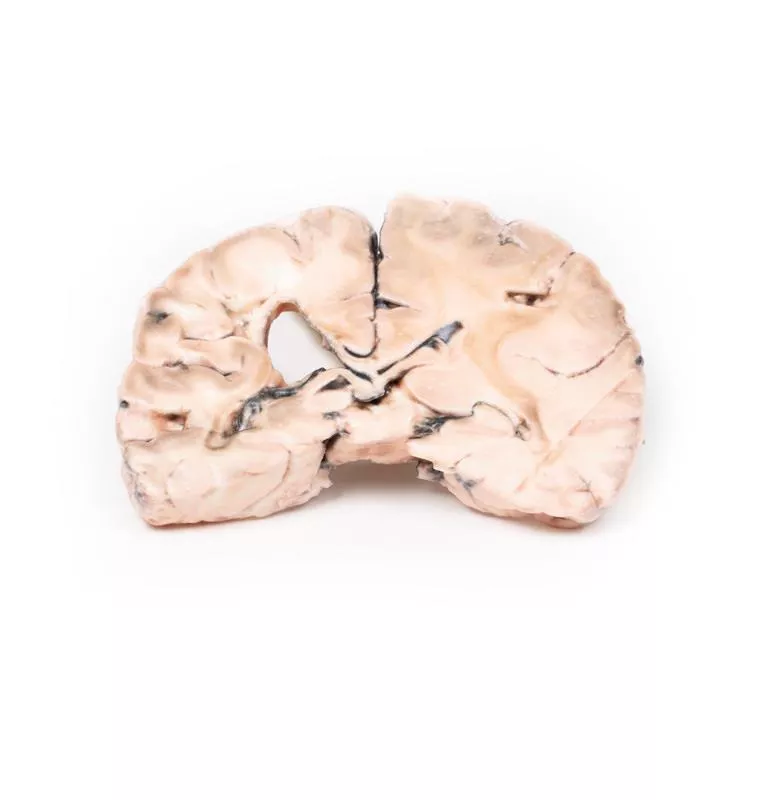
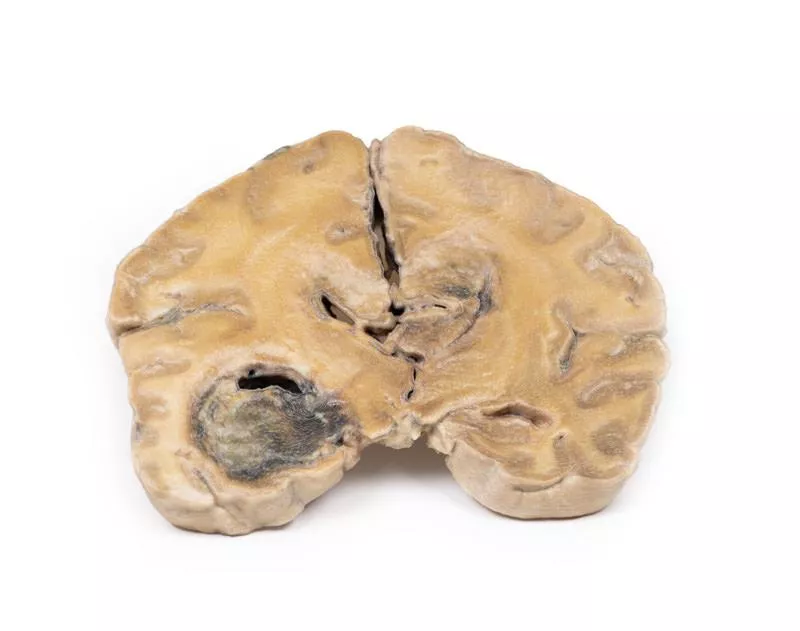
Left cerebral infarct
Clinical HistoryThe patient was a 51-year-old woman who had suffered a cerebrovascular accident two years before death, resulting in left-sided hemiplegia. At autopsy, she showed severe generalised atherosclerosis and an old myocardial infarction in the left ventricle with an overlying mural thrombus.PathologyA coronal section of the brain reveals irregular cystic cavities in the region supplied by the right middle cerebral artery, consistent with an old infarct. The cavity walls are yellow and partially collapsed. There is compensatory dilatation of the left lateral ventricle. The arteries below the mammillary bodies appear moderately atheromatous, though this is not easily seen macroscopically. Further InformationGiven the history of cardiac disease and a mural thrombus, the cerebral infarct was most likely caused by a thromboembolus originating from the heart.
Cerebral Haemorrhage, secondary to Acute Myeloid Leukaemia
Clinical HistoryA 22-year-old male presented with a two-week history of malaise, weight loss and unexplained bruising. He later developed productive cough and fever. Shortly after hospital admission for further tests, he suddenly lost consciousness and died within minutes.PathologyThis horizontal brain section shows the superior surface with two large haemorrhages in the right frontal and parietal lobes (each approx. 5 cm), as well as multiple smaller haemorrhages in the white matter bilaterally. This presentation is consistent with multiple intraparenchymal haemorrhages in a patient with acute myeloid leukaemia (AML). Further InformationIntraparenchymal brain haemorrhages result from rupture of small blood vessels in the brain and often present with sudden neurological decline. In AML, bone marrow failure due to immature blast accumulation leads to thrombocytopaenia, increasing the risk of spontaneous bleeding. Intracranial haemorrhage is the second most common cause of death in AML after infection. A severe bleeding disorder, disseminated intravascular coagulation (DIC), can also occur. Treatment options depend on the severity and may include haematoma evacuation, seizure control and management of intracranial pressure. Mortality for intracerebral haemorrhage is high, especially within the first 48 hours.
Glioblastoma multiforme
Clinical HistoryOver a 3-year period, a 57-year-old woman experienced intermittent frontal headaches and memory disturbances that progressed to psychiatric symptoms, vomiting, and meningeal signs. Localising neurological signs appeared only late in the disease course.Pathology A coronal section of the cerebral hemisphere reveals a round, haemorrhagic, variegated tumour in the left temporal lobe. Tumour tissue extends across the midline, replacing the corpus callosum and nearly obliterating the ventricular system. Further sections confirmed these lesions are part of one massive tumour. Further Information Gliomas are the second most common CNS cancer after meningiomas. These tumours resemble normal macroglial cells—astrocytes, oligodendrocytes, and ependymal cells—and arise from progenitor cells differentiating along these lines. Glioblastoma multiforme (GBM), a grade IV astrocytoma, can develop de novo or from lower-grade gliomas. Histologically, GBMs feature necrosis surrounded by anaplastic cells and hyperplastic blood vessels. GBMs are more frequent in males and typically diagnosed in the 6th decade. Risk factors include neurofibromatosis type 1, Li-Fraumeni syndrome, and prior brain radiotherapy. Symptoms depend on tumour location and include persistent headaches, visual disturbances, vomiting, appetite loss, mood and personality changes, cognitive decline, new seizures, and speech difficulties. Diagnosis relies on CT and MRI. About 50% of GBMs involve more than one hemisphere and often invade ventricular walls or meninges, occasionally reaching the CSF. Metastases outside the CNS are rare. Tumour growth causes cerebral oedema and increased intracranial pressure. These aggressive tumours have a median survival of around 3 months if untreated. Treatment includes surgery, radiation, and chemotherapy.
Berry Aneurism of Basilar Artery
Clinical HistoryA 37-year-old patient presented with headache, vomiting, and disorientation after head trauma. CT revealed dilated lateral ventricles and a mass projecting into the third ventricle. A shunt was placed for hydrocephalus. Angiography identified a partially thrombosed 1 × 1 cm basilar artery aneurysm. The aneurysm enlarged over time, and multiple surgical attempts, including ligation and shunt revisions, were unsuccessful. The patient remained unconscious and later died.PathologyThis mid-sagittal brain section (1 cm thick) shows a large, dark berry aneurysm (5 × 2 cm) from the basilar artery, eroding into the midbrain and pons, and compressing the third ventricle. The aneurysm is filled with a laminated thrombus, with blood visible in the third ventricle and signs of leakage. A mucoid degeneration (0.4 cm) is present in the pons. The lateral view shows ventricular dilatation, blood staining, and haemorrhagic infarction of the caudate nucleus, along with meningeal discolouration consistent with subarachnoid haemorrhage. Further InformationIntracranial aneurysms occur in ~3.2% of the population, with rupture rates of 7.9 per 100,000 person-years. Posterior circulation aneurysms are less common and typically found at basilar, vertebral, or cerebellar artery junctions. Symptoms arise from subarachnoid haemorrhage or mass effect. Complications include raised intracranial pressure, hydrocephalus, re-bleeding, and vasospasm. Treatment options include surgical and endovascular interventions.
Glioma grade 3-4, causing papilloedema
Clinical HistoryThe patient was a 24-year-old woman who initially presented with an abnormal EEG following a single epileptic seizure. Six months later, she developed blurred vision and headaches. Ophthalmoscopy revealed bilateral papilloedema, though no focal neurological signs were found. Imaging identified a space-occupying mass, biopsied and diagnosed as a Grade III–IV glioma. She underwent radiotherapy, but a month later developed weakness in her left arm and leg. Shortly thereafter, she was admitted with drowsiness and vomiting and died soon after.PathologyThe specimen reveals a large intracerebral tumour, obliterating the lateral ventricles and the inner two-thirds of the internal capsule and basal ganglia on the right. The tumour crosses the corpus callosum and distorts the aqueduct. It is relatively well-demarcated and highly vascular, with extensive haemorrhage and necrosis, giving it a mottled appearance.
Meningioma
Clinical HistoryA 68-year-old woman presented with new-onset seizures and was diagnosed with epilepsy. A collateral history revealed a gradual personality change. Several months later, she died from a myocardial infarction.PathologyThe tumour is located between the two frontal lobes, compressing them. It has a pinkish cut surface with yellow areas indicating necrosis and is attached anteriorly to the dura mater. This represents a typical meningioma. Further InformationMeningiomas are among the most common tumours associated with the central nervous system, though they originate from the arachnoid cells of the meninges (not the CNS itself). They are often attached to the dura or its folds (e.g. falx cerebri, tentorium cerebelli) and are typically slow-growing and benign.Symptoms depend on tumour size and location and may include seizures, personality changes, sensory disturbances, or signs of increased intracranial pressure. Many meningiomas remain asymptomatic.Treatment ranges from depending on clinical presentation and tumour type.Meningiomas are rare in children. The median age at diagnosis is 65, and they are more common in women (3:2). Ionising radiation, especially cranial radiotherapy, increases the risk. The strongest genetic predisposition is seen in neurofibromatosis type 2 (NF2), a dominant disorder caused by NF2 gene mutations on chromosome 22, often resulting in multiple nervous system tumours.
Pituitary Adenoma
Clinical HistoryA 29-year-old male presented with a 22-month history of headaches and blurred vision. Examination revealed a bitemporal hemianopia and a left sixth nerve palsy. Skull X-ray showed erosion of the sphenoid body, with some of the dorsum sellae and anterior clinoid process intact. Carotid angiography demonstrated upward and lateral displacement of the anterior and middle cerebral arteries. Pneumoencephalography showed upward displacement of the lateral and third ventricles. A craniotomy was performed, but the patient died immediately after surgery.PathologyThe pituitary gland has been completely replaced by a 4 cm round tumour, seen in a sagittal brain section to the right of the falx cerebri. The cut surface of the tumour is pale brown and homogeneous, with a small area of haemorrhage likely caused by surgical trauma. The tumour caused upward displacement of the midbrain and erosion of the sphenoid bone, enlarging the sella turcica. The optic chiasma is compressed. Histological diagnosis: chromophobe adenoma of the anterior pituitary. Further InformationThis case used now outdated methods such as pneumoencephalography. Today, a CT followed by a brain MRI would be standard. Pituitary adenomas are the most common pituitary tumours, typically affecting adults between 35 and 60 years. Clinical signs relate to mass effect—including increased intracranial pressure, bony erosion, and optic chiasma compression—as well as hormonal activity. About 75% are functioning adenomas (e.g., prolactin, growth hormone, or ACTH secretion), while non-functioning tumours may present later and cause hypopituitarism due to compression of the remaining gland.
Metastatic Adenocarcinoma in the Brain
Clinical HistoryA 56-year-old male underwent a total gastrectomy and splenectomy for gastric adenocarcinoma. Over two months, he developed a progressively unsteady gait, left hand weakness, and frontal headaches with nausea and vomiting. Imaging revealed a right frontal lobe lesion. Following craniotomy and resection, pathology confirmed a metastatic gastric adenocarcinoma. The patient's condition worsened with jaundice, papilloedema, and declining consciousness due to increased intracranial pressure. Repeat imaging showed recurrence of the brain lesion and liver metastases. He died 9 months after gastrectomy.PathologyThis coronal brain section reveals a well-defined, variegated pink-grey tumour in the right frontal lobe, involving both grey and white matter. There is visible compression of the right lateral ventricle and midline shift caused by the mass. Further InformationStomach cancer is a leading cause of cancer-related death worldwide. Risk factors include male sex, diet, smoking, and Helicobacter pylori infection. Gastric adenocarcinoma most commonly metastasises to the liver, peritoneum, lungs, and bones. Brain metastases are rare (weniger als 1 %) and typically occur in widespread disease, carrying a poor prognosis. Palliative care may include surgery, radiotherapy, steroids, chemotherapy, or combinations thereof.
Ventriculitis, Secondary to Septicaemia
Clinical HistoryA 50-year-old male with alcoholism was admitted with a 2-week history of weakness and shortness of breath. He initially presented with productive cough, chest pain, and blood-stained sputum. On examination, he was febrile, cyanosed, and drowsy, with grunting respiration and a friction rub over the right lower lobe. His condition worsened progressively. Shortly before death, a lumbar puncture yielded green opalescent fluid. Blood cultures confirmed Streptococcus pneumoniae.PathologyThis is a case of ventriculitis, alongside pneumococcal meningitis and right basal pneumonia. A horizontal brain section shows both lateral ventricles with a thickened, rough ependymal lining and cellular debris near the choroid plexus and anterior horn. Structures like the caudate nucleus, lentiform nucleus and internal capsule are visible. Histology revealed extensive neutrophilic infiltration of the subarachnoid space, vascular wall involvement, and cerebral parenchymal inflammation causing haemorrhage and necrosis. Further InformationVentriculitis is a rare complication of intracranial infection. In adults, it usually occurs secondarily to surgery or trauma rather than primary meningitis. Common pathogens include staphylococci and resistant Gram-negative bacilli. In infants under 6 months, incidence is higher. Symptoms may mimic hydrocephalus due to aqueductal obstruction. Diagnosis relies on CSF analysis and imaging (CT, MRI). Treatment involves prolonged intravenous antibiotics that can penetrate CSF and brain tissue.
Cerebral Arterio-Venous Malformation
Clinical HistoryThis 58-year-old patient died due to post-operative complications following transurethral resection of the prostate. He had experienced two episodes of transient neurological deficits at the ages of 28 and 35. At 50, he developed a permanent hemiparesis affecting the left leg, primarily the ankle.PathologyThis coronal brain slice through the parietal lobes reveals a 4 cm lesion in the medial right hemisphere, extending from the cortical surface to the lateral ventricle. The abnormal area consists of tortuous vascular channels and interspersed tissue. Histology confirmed an arteriovenous malformation (AVM) with glial tissue surrounding vessels of both arterial and venous character. Further InformationCerebral AVMs can cause a range of symptoms such as headaches, seizures, and cranial nerve deficits, though some patients remain asymptomatic. In serious cases, vessel rupture may lead to intracranial haemorrhage, resulting in loss of consciousness, nausea, vomiting, and vision problems. Neurological deficits like hemiparesis or aphasia may occur depending on the bleed location. Ruptured AVMs carry significant risks of both mortality and long-term disability.
Intracranial space-occupying lesion
Clinical HistoryA 56-year-old woman with a 6-month history of intermittent headaches and vomiting was admitted to hospital in a comatose state following a grand mal seizure. She did not regain consciousness.Pathology This coronal brain section reveals that the brain has been compressed laterally and downward due to a large intracranial mass on the right side, likely a meningioma (though the tumour itself is not present in the section). The anterior view shows a midline shift with subfalcine herniation of the cingulate gyrus. The posterior view displays haemorrhages of varying ages in the temporal lobe and pons, which are typical for a supratentorial mass lesion. There is also noticeable ventricular asymmetry. Further Information A space-occupying meningioma can exert pressure on brain tissue, resulting in atrophy and displacement, which in turn may affect cranial nerve function, blood flow, and normal brain processes. Common symptoms may include: - Seizures – such as myoclonic (brief muscle jerks or spasms) or tonic-clonic (loss of consciousness, muscle rigidity, followed by convulsions and potential loss of body control). - Sensory disturbances – changes in vision, smell, or hearing without loss of consciousness.The presentation can vary depending on the tumour’s location.
Craniopharyngioma
Clinical HistoryA 62-year-old woman presented with disorientation to time, place, and person. Physical examination showed no localized neurological deficits. Imaging revealed a space-occupying lesion in the floor of the 3rd ventricle. During surgery, tissue was removed but complete excision was not possible. Histology confirmed the diagnosis of Craniopharyngioma. Postoperatively, the patient developed complex metabolic disturbances likely originating from the hypothalamus. Her condition worsened gradually, and she died 10 weeks after admission following gastric aspiration.PathologyThe sagittally sectioned brain shows a pink-grey, ovoid tumour measuring 2.5 x 1.5 cm located in the hypothalamic region. The tumour is encapsulated except at the ventral pole where surgery had removed tissue. The cut surface reveals a microcystic or spongy appearance. It distorts the 3rd ventricle and blocks the Foramen of Munro. The optic chiasm is displaced downward. A previous ventriculo-atrial shunt prevented dilation of the lateral ventricles despite this obstruction. Further InformationCraniopharyngiomas account for 1-3% of all brain tumours and 5-10% in children, with two age peaks: 5-14 years and 50-75 years. Higher incidence is reported in Japan and parts of Africa. These epithelial tumours arise mainly from the pituitary stalk but can also originate in the sella turcica, optic system, or third ventricle. They often have both solid and cystic components, the cysts containing cholesterol crystals. Two main types exist: adamantinomatous and papillary, differing in histology and genetics though prognostic relevance remains unclear. Treatment involves surgical resection and radiation therapy to address residual disease. Prognosis depends on tumour control and complications from local and endocrine effects.
Human body replicas to improve teaching!
Erler-Zimmer's groundbreaking Anatomy Series features a unique and unrivalled collection of colourised human body replicas specifically designed to enhance teaching and learning. This premium collection of highly accurate human anatomy has been created directly from radiological data or real specimens using the latest imaging techniques. The 3D Human Anatomy Series offers a cost-effective way to meet your specific teaching and demonstration needs across the curriculum in medicine, health sciences and biology. A detailed description of the anatomy represented in each 3D printed specimen is included. What are the advantages of the Monash 3D Anatomy Series compared to plastic models or real human plastinates?
Each body replica has been carefully developed from selected radiological patient data or dissected human bodies of the highest quality, chosen by a highly skilled team of anatomists at Monash University's Human Anatomy Teaching Centre, to represent clinically important areas of anatomy in a quality and detail not possible with conventional models - it is real anatomy, not stylised. Each body replica has been rigorously checked by the highly qualified team of anatomists at Monash University's Human Anatomy Teaching Centre to ensure the anatomical accuracy of the final product. The body replicas are not real human tissue and are therefore not subject to any restrictions on transport, import or use in educational institutions that do not have permission to use cadavers. The
exclusive 3D Anatomy Series avoids these and other ethical issues that arise when dealing with plastinated human remains.